A. Introduction to Behavioral Health Transformation
In recent years, California has undertaken historic efforts to re-envision the state’s publicly funded mental health and substance use disorder (SUD) services, with a special focus on county-administered specialty mental health and substance use disorder services. In March 2024, voters approved Proposition 1 to reform the Mental Health Services Act (MHSA) and fund needed behavioral health facility infrastructure through a general obligation bond. The efforts to implement Proposition 1 are referred to as Behavioral Health Transformation (BHT).
The primary goals of BHT are to improve access to care, increase accountability and transparency for publicly funded, county-administered behavioral health services, and expand the capacity of behavioral health care facilities across California. Under BHT, county reporting will be uniform to allow for comprehensive and transparent reporting of the Behavioral Health Services Act (BHSA) funding in relation to all public local, state, and federal behavioral health funding.
BHT builds upon and aligns with other major behavioral health initiatives in California including the California Advancing and Innovating Medi-Cal (CalAIM) initiative, the California Behavioral Health Community-Based Organization Networks of Equitable Care and Treatment (BH-CONNECT) initiative, the Children and Youth Behavioral Health Initiative (CYBHI), Medi-Cal Mobile Crisis services, the Behavioral Health Bridge Housing program, the Community Assistance, Recovery, and Empowerment (CARE) Act, Lanterman-Petris-Short Conservatorship reforms (WIC section 5402, subdivision (g)(2)), 988 expansion, and the Behavioral Health Continuum Infrastructure Program (BHCIP).
California continues to face behavioral health challenges impacted by many factors, including but not limited to the lack of affordable housing and increasing homelessness, the behavioral health workforce shortage, a youth mental health crisis, an older adult mental health crisis, and a shortage of culturally-responsive and diverse care. Many of these challenges make it difficult for individuals to navigate California’s behavioral health care delivery systems and access services at the right time and in the right place. For example, 2022 survey research suggests that 23.5 percent of adult Californians across all payers living with a mental illness reported they did not receive the treatment they needed.
A.1 Bond
In addition to reforming the MHSA, Proposition 1 includes the Behavioral Health Infrastructure Bond Act of 2023. This bond authorizes $6.38 billion to build new behavioral health treatment beds and supportive housing units to help serve more than 100,000 people annually. This investment creates new, dedicated housing for people experiencing or at risk of homelessness who have behavioral health needs, with a dedicated investment to serve veterans. These settings will provide Californians experiencing behavioral health conditions with places to stay while safely stabilizing, healing, and receiving ongoing support.
-
Department of Health Care Services (DHCS) will administer $4.4 billion of these funds to provide grants to public and private entities for behavioral health treatment and residential settings. $1.5 billion of the funds administered by DHCS will be awarded only to counties, cities, and tribal entities (with $30 million set aside for tribes).
-
The California Department of Housing and Community Development (HCD) will administer up to $2 billion to support permanent supportive housing for individuals, including veterans, at risk of or experiencing homelessness and behavioral health challenges.
A.2 Behavioral Health Continuum Infrastructure Program
In 2021, DHCS was authorized to establish the Behavioral Health Continuum Infrastructure Program (BHCIP) and award $2.1 billion in funding to construct, acquire, and expand properties and invest in mobile crisis infrastructure related to behavioral health. DHCS has been releasing these funds through multiple grant rounds targeting various gaps in the state’s behavioral health facility infrastructure.
The Behavioral Health Bond Act of 2023 leverages the success of BHCIP and authorizes DHCS to award up to $4.4 billion for BHCIP competitive grants. Please refer to the BHCIP webpage for the latest information.
B. Overview of the Behavioral Health Services Act
B.1 Behavioral Health Services Act Goals
The Behavioral Health Services Act (BHSA) is the first major structural reform of the Mental Health Services Act (MHSA) since it was passed in 2004. The MHSA imposed a 1 percent tax on personal income over $1 million. Counties and two city-operated mental health authorities receive these funds monthly to provide community-based mental health services. The MHSA was designed to serve individuals with serious mental illness (SMI) (WIC section 5600.3, subdivision (b)(2)) and individuals that may be at risk of developing serious mental health conditions. The MHSA created a broad continuum of prevention, early intervention, innovative programs, services, and infrastructure, technology, and training elements. MHSA has been a crucial resource to increase access to mental health services for all eligible populations.
The reforms within the BHSA expand the types of behavioral health supports available to Californians who are eligible for services and are in need by focusing on historical gaps and emerging policy priorities. The key opportunities for transformational change within the BHSA include:
-
Reaching and Serving High Need Priority Populations
-
Restructures funding allocations for the BHSA program components by focusing allocations on the areas of most significant need among Californians, including individuals across the lifespan at risk of or experiencing justice and system involvement, homelessness, and institutionalization.
-
Prioritizes early intervention, especially for children and families, youth, and young adults, to provide early linkage to services and prevent mental health conditions, co-occurring disorders, and substance use disorders from becoming severe and/or disabling.
-
Prioritizes serving individuals experiencing homelessness or at risk of homelessness, especially individuals and families experiencing long-term homelessness. The BHSA dedicates revenue for counties to assist those with severe behavioral health needs to be housed and provides a path to long-term recovery, including one-time and allowable ongoing capital to build more housing options.
-
Updates Full Service Partnerships (FSP) requirements to better serve individuals with the most significant needs by requiring FSP programs to include specified, evidence-based delivery models, community-defined evidence practices, and standardized levels of care.
-
Aligns with initiatives aimed at improving care for Medi-Cal members living with significant behavioral health needs such as the California Advancing and Innovating Medi-Cal (CalAIM) initiative, the California Behavioral Health Community-Based Organization Networks of Equitable Care and Treatment (BH-CONNECT) initiative, the Children and Youth Behavioral Health Initiative (CYBHI), Medi-Cal Mobile Crisis Services, the Behavioral Health Bridge Housing program, the Community Assistance, Recovery, and Empowerment (CARE) Act, Lanterman-Petris-Short Conservatorship reforms (WIC section 5402, subdivision (g)(2)), 988 expansion, and the Behavioral Health Continuum Infrastructure Program (BHCIP).
-
Increasing Access to Substance Use Disorder Services, Housing Interventions, and Evidence-Based and Community-Defined Practices, and Building the Behavioral Health Workforce
-
Expands the categories of services that may be funded with BHSA dollars to include treatment for substance use disorders, regardless of the presence of a co-occurring mental health condition.
-
Provides ongoing funding for counties to assist people living with significant mental health conditions, substance use disorder needs and co-occurring behavioral health needs with housing and provides a path to long-term recovery, including one-time and allowable ongoing capital to build more housing options.
-
Increases investments in the behavioral health workforce including efforts to support more culturally, linguistically, and age-appropriate care by building a more representative workforce.
-
Requires implementation of specified evidence-based and community-defined evidence practices to improve outcomes for youth and adults with complex behavioral health conditions.
-
Focusing on Outcomes, Transparency, Accountability, and Equity
-
Requires counties to complete a county Integrated Plan for behavioral health services and outcomes, which will include information on all local behavioral health funding and services, including Medi-Cal and non-Medi-Cal specialty behavioral health programs and funding streams.
-
Requires counties to complete an annual county Behavioral Health Outcomes, Accountability, and Transparency Report (BHOATR) to provide public visibility into county spending, disparities, and results.
-
Utilizes data through the lens of health equity to identify racial, ethnic, age, gender, and other demographic disparities and inform disparity reduction efforts.
-
County BHSA programs must include culturally responsive and linguistically appropriate interventions. These interventions must be able to reach underserved cultural populations and address specific barriers related to racial, ethnic, cultural, language, gender, age, economic, or other disparities in mental health and substance use disorder treatment services access, quality, and outcomes.
B.2 Timeline for Implementation
Table B.2.1. Timeline for Implementation
|
Requirement |
Effective Date |
|
Counties Submit Draft FY 2026-2029 County Integrated Plan to DHCS with County Administrative Officer (CAO) Approval |
No later than March 31, 2026 |
|
Counties Submit Final FY 2026-2029 County Integrated Plan to DHCS County Board of Supervisors Approve Final Fiscal Year (FY) 2026-2029 County Integrated Plan |
No later than June 30, 2026 |
|
County Integrated Plans Are Effective |
July 1, 2026 |
|
Counties Submit Draft 2027-2028 County Annual Update to DHCS with CAO Approval |
No later than March 31, 2027 |
|
Counties Submit Final FY 2027-2028 County Annual Update to DHCS County Board of Supervisors Approve Final FY 2027-2028 County Annual Update |
No later than June 30, 2027 |
|
Submit Draft FY 2026-2027 County Behavioral Health Outcomes, Accountability, and Transparency Report (BHOATR) |
January 30, 2028 |
|
Submit Final FY 2026-2027 County Behavioral Health Outcomes, Accountability, and Transparency Report (BHOATR) |
January 30, 2029 |
B.3 Eligible Populations
Eligible children and youth means persons who are 25 years of age or under who meet either of the following:
-
Meet SMHS access criteria specified in subdivision (d) of WIC section 14184.402 and implemented in SMHS guidance (includes individuals 21-25 years of age who meet this criteria) OR
-
Have at least one diagnosis of a moderate or severe substance use disorder from the most current version of the Diagnostic and Statistical Manual of Mental Disorders (DSM) for Substance-Related and Addictive Disorders, with the exception of tobacco-related disorders and non-substance-related disorders (WIC section 5891.5, subdivision (c)(1)).
Eligible adults and older adults mean persons who are 26 years of age or older who meet either of the following:
-
Meet SMHS access criteria specified in WIC section 14184.402, subdivision (c) and implemented in DHCS guidance (only applies to individuals 26 years of age and older) OR
-
Have at least one diagnosis of a moderate or severe substance use disorder from the most current version of the Diagnostic and Statistical Manual of Mental Disorders (DSM) for Substance-Related and Addictive Disorders, with the exception of tobacco-related disorders and non-substance-related disorders (WIC section 5891.5, subdivision (c)(1)).
Priority Populations
In addition to defining the populations eligible for services, the BHSA also requires counties to prioritize BHSA services for the populations listed below (WIC section 5892, subdivision (d)). While counties must prioritize BHSA services for the priority populations listed below, access to BHSA services is not limited to these priority populations. At-risk populations should be identified by counties based on local need and local planning processes, except for the criteria for at-risk of homelessness which can be found in the Housing Interventions chapter and below.
Eligible children and youth who satisfy one of the following:
-
Are chronically homeless or experiencing homelessness or at risk of homelessness
-
Are in, or at risk of being in, the juvenile justice system
-
Are reentering the community from a youth correctional facility
-
Are in the child welfare system pursuant to WIC sections 300, 601, or 602
-
Are at risk of institutionalization (The DHCS ECM Guide defines institutionalization as “broad and means any type of inpatient, Skilled Nursing Facility, long-term, or emergency department setting.”)
Eligible adults and older adults who satisfy one of the following:
-
Are chronically homeless or experiencing homelessness or at risk of homelessness
-
Are in, or at risk of being in, the justice system
-
Are reentering the community from state prison or county jail
-
Are at risk of conservatorship
-
Are at risk of institutionalization (The DHCS ECM Guide defines institutionalization as “broad and means any type of inpatient, Skilled Nursing Facility, long-term, or emergency department setting.”)
For additional information about criteria or priority populations for Full Service Partnerships and Housing Interventions, including the definition for “chronically homeless”, please refer to the corresponding sections within this manual.
C. Statewide Vision for Behavioral Health Quality and Equity
The state is committed to boldly taking action to provide Californians with quality, culturally responsive behavioral health services when, how, and where they need them. It will take cross-system collaboration and partnership across service delivery systems to address the statewide behavioral health goals discussed in this Policy Manual. DHCS, county behavioral health, Medi-Cal Managed Care Plans (MCPs), commercial plans, commercial plan regulators, and other key delivery system partners such as child welfare, public health, schools and others will share responsibility for improving the well-being of Californians in need of behavioral health services.
C.1 A Population Health Approach to Behavioral Health
The Behavioral Health Transformation presents a historic opportunity to transform behavioral health service delivery by:
-
Taking a population health approach to align expectations across California’s behavioral health delivery system.
-
Establishing a vision for quality and equity and setting statewide goals to drive progress across the behavioral health delivery system.
-
Using data to support continuous quality improvement.
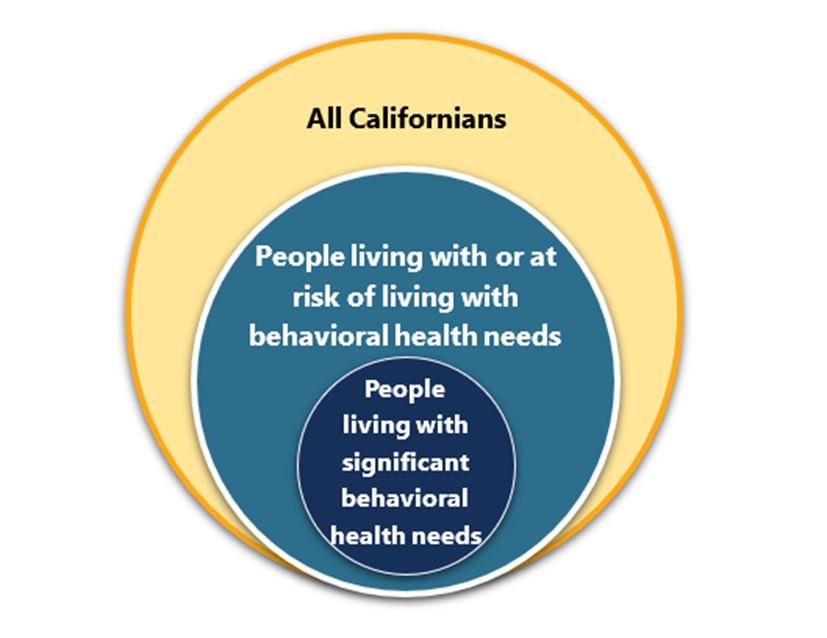
A population health approach aims to address these gaps in access to care and connect individuals to the right services, in the right place, and at the right time.
A population health approach for the behavioral health delivery system:
-
Considers the entire population eligible for public behavioral health services, not just those currently receiving behavioral health services and those seeking care (shown in Figure 2.C.3).
-
Deploys whole-person care interventions, including addressing social drivers of health, which are the environments in which people are born, live, learn, work, play, worship, and age that affect a wide range of health functioning and quality of life outcomes and risk factors.
-
Coordinates across service delivery systems, including cross-system collaboration and partnership across county behavioral health, Medi-Cal MCPs, commercial plans, commercial regulators, public health, and other key service delivery partners.
-
Uses data to:
-
Identify underserved and unserved population groups for targeted interventions, including BHSA priority populations.
-
Improve quality across the behavioral health care continuum.
-
Monitor effectiveness of interventions across populations.
-
Support continuous improvement.
-
Identify and track racial and ethnic disparities in behavioral health outcomes.
-
Like the Population Health Management (PHM) Program for Medi-Cal MCPs implemented in January 2023, a population health approach to behavioral health will reorganize and strengthen existing contract requirements, particularly requirements related to collaboration across the delivery system, and is targeted to the delivery system that DHCS oversees.
DHCS is working to align priorities and desired outcomes across the behavioral health delivery system, payers (e.g., Medi-Cal MCP Non-Specialty Mental Health Services (NSMHS) and Medi-Cal Specialty Mental Health Services (SMHS)), initiatives and funding sources (e.g., BHSA, Medi-Cal federal financing participation and non-federal share, and Realignment and Block Grants), while still allowing for initiative-specific goals.
As outlined in WIC section 5963.02, subdivision (c)(3)(A), each county shall develop an Integrated Plan (IP) and annual update (AU) aligned with statewide behavioral health goals and their associated measures. DHCS has defined statewide population behavioral health goals to identify the improvements that counties and the state should be working towards together across the behavioral health delivery system.
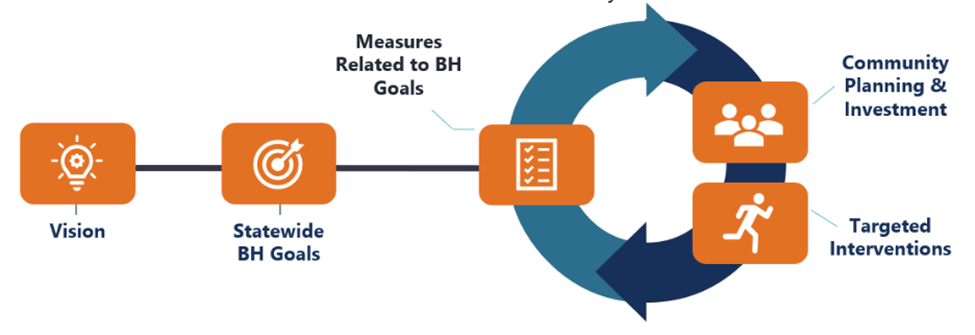
Specifically, DHCS is partnering with counties to participate in a cycle of continuous improvement to drive progress on the statewide behavioral health goals (shown in Figure 2.C.4):
-
Establish statewide behavioral health goals.
-
In consultation with behavioral health stakeholders and subject matter experts, identify at least one measure for each behavioral health goal.
-
Deliver measures to county behavioral health and Medi-Cal MCPs describing their performance on the statewide behavioral health goals and enabling them to:
-
Utilize data on measure performance during the Community Planning Process (detailed in Chapter 3, section 3.B the Policy Manual) to work with key stakeholders to address the statewide population behavioral health goals;
-
Make investments (such as workforce and infrastructure investments) that are expected to advance the goals; and
-
Implement targeted interventions that are expected to improve progress on the goals.
-
DHCS recognizes that shifting to a coordinated, data-driven, population behavioral health approach will take time. As with the PHM Program, DHCS will phase in requirements and provide technical assistance to counties and other key stakeholders.
C.2 Statewide Population Behavioral Health Goals
DHCS, in consultation with behavioral health stakeholders and subject matter experts, has identified 14 statewide behavioral health goals focused on improving wellbeing (e.g., quality of life, social connection) and decreasing adverse outcomes (e.g., suicides, overdoses). These behavioral health goals (shown in Figure 2.C.5) will inform state and county planning and prioritization of BHSA resources, and DHCS will continuously assess statewide and county progress toward these goals under BHT.
Note that health equity, defined as the “reduction or elimination of health disparities, health inequities, or other disparities in health that adversely affect vulnerable populations”, will be incorporated in each of the statewide behavioral health goals. DHCS will endeavor to provide measures that can be stratified (e.g., by demographics such as age group and race/ethnicity, etc.) to enable visibility into disparities. In addition to identifying disparities, DHCS will ask counties and Medi-Cal Managed Care Plans (MCPs) to address disparities and DHCS will consider disparities when developing accountability measures.

DHCS selected these goals based on their strong indication of the health and wellbeing of Californians living with significant behavioral health needs. In alignment with the mission of BHT to improve behavioral health for Californians, the statewide population behavioral health goals lay out the vision that the state, counties, MCPs, and other key stakeholders must work towards to improve the overall well-being of Californians who are living with behavioral health needs (see Tables 2.C.1 and 2.C.2 for the goals’ definitions and rationale for inclusion).
Table 2.C.1. Statewide Population Behavioral Health Goals: Goals for Improvement
– Definition and Rationale
|
Goals for Improvement |
Definition and Rationale |
|
Care experience |
Care experience refers to the range of interactions and quality of care that patients have and receive from the healthcare system that can impact level of engagement and length of treatment. Improving the care experience (e.g., care is culturally congruent and responsive, trauma-informed, etc.) in California’s behavioral health delivery system is important; positive experiences with care can lead to greater treatment engagement, adherence, and remaining in treatment longer, leading to positive health outcomes. |
|
Access to care |
Access to care is defined as the timely and appropriate use of health services to achieve the best possible health outcomes, inclusive of all modalities. Improving Californians’ access to care is necessary for improving outcomes. Compliance with provider availability as outlined in network adequacy requirements, strategies for navigating the complex care delivery system, and improving wait times for appointments will enable Californians to better access the right care at the right time. |
|
Prevention and treatment of co-occurring physical health conditions |
Co-occurrence in this goal refers to the prevention or treatment of a physical health condition in an individual with an existing BH condition. An integrated care approach that addresses both behavioral and physical health needs of individuals can lead to earlier treatment of uncontrolled chronic physical health conditions. |
|
Quality of life |
Quality of life is defined as an individual’s “perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns.” Individuals living with behavioral health conditions face challenges from symptoms and associated stigma, which can negatively impact daily functioning, wellbeing, and overall quality of life. |
|
Social connection |
Social connection refers to the degree to which an individual has the number, quality, and variety of relationships that they want to feel and have belonging, support, and care. Establishing and maintaining supportive relationships is vital for preventing and managing significant behavioral health needs along with other behavioral health conditions associated with loneliness and isolation. |
|
Engagement in school |
In this context, engagement refers to the degree of attention, curiosity, interest, passion, and optimism that an individual has towards school and related activities, including their enrollment and participation in as well as graduation from school. Enhancing engagement through prevention and treatment of behavioral health conditions can enable individuals to participate actively and meaningfully, leading to improvements in quality of life, independence, and wellbeing. |
|
Engagement in work |
Similar to above, engagement refers to the degree of attention, curiosity, interest, passion, and optimism that an individual has towards work and related activities. Enhancing engagement in the workplace as part of paid employment or unpaid work through prevention and treatment of behavioral health conditions can enable individuals to participate actively and meaningfully, leading to improvements in job performance, productivity, job satisfaction, and overall personal wellbeing. |
Table 2.C.2. Statewide Population Behavioral Health Goals: Goals for Reduction
– Definition and Rationale
|
Goals for Reduction |
Definition and Rationale |
|
Suicides |
Suicide, including suicide attempts is defined as death or non-fatal, potentially injurious harm caused by self-directed injurious behavior with the intent to die as a result of the behavior. (DHCS does not have a formal definition for “suicide,” but acknowledges it as a complex public health challenge involving many biological, psychological, social, and cultural determinants. More on its program can be found in the DHCS Suicide Prevention Fact Sheet). Strengthening California’s behavioral health delivery system and providing targeted and tailored suicide prevention efforts is critical for reducing California’s suicide rate. |
|
Overdoses |
A drug-related overdose can occur when a toxic amount of a drug, or combination of drugs, including prescription, illicit, or alcohol, overwhelms the body. In California, drug-related overdose deaths have doubled since 2017, reaching 10,898 in 2021, with the greatest impact among racial and ethnic minorities, and individuals experiencing homelessness, unemployment, and incarceration. |
|
Untreated behavioral health conditions |
Untreated behavioral health conditions refer to an individual’s behavioral health condition that has not been diagnosed or attended to with appropriate and timely care. Living with untreated behavioral health conditions can lead to worsening symptoms, diminished quality of life, unemployment, reduced educational attainment, homelessness, and higher risk of severe outcomes such as suicide or self-harm. |
|
Institutionalization |
Minimize time in institutional settings by ensuring timely access to community-based services across the care continuum and in a clinically appropriate setting that is least restrictive. Reducing institutionalization entails maximizing community integration and making supportive housing options with intensive, flexible, voluntary supports and services available to all individuals who would benefit. Stays in institutional settings are sometimes clinically appropriate and therefore the goal is not to reduce institutionalization stays to zero. |
|
Homelessness |
Homelessness is defined below in Chapter 7, Section C.4.1.1 of the Housing Interventions chapter. Addressing the increase in statewide homelessness is crucial to ensuring unhoused individuals living with significant behavioral health needs receive regular access to behavioral health treatment and safe and stable housing where they can recover. |
|
Justice-Involvement |
Reducing justice involvement refers to reducing adults and youth living with behavioral health needs who are involved in the justice system - including those who have been arrested, are living in, who are under community supervision, or who have transitioned from a state prison, county jail, youth correctional facility, or other state, local, or federal carcel settings where they have been in custody of law enforcement authorities. More than 50 percent of incarcerated individuals living with a behavioral health condition. While incarcerated, justice-involved individuals living with behavioral health needs have limited access to treatment. Formerly incarcerated individuals are more likely to experience poor health outcomes, including higher risk for injury and death due to violence, overdose, and suicide. Promoting coordinated systems of care between the legal system and behavioral health plans and providers can have an impact on reducing justice involvement and improving outcomes for those who are justice-involved. |
|
Removal of children from home |
Removal of children from home, specifically those with an open child welfare status, refers to when children may be removed from their home due to abuse and/or neglect. Providing early intervention and intensive BH services to parents and additional members of the family unit living with a behavioral health condition can prevent family disruption and improve child welfare outcomes, as children are less likely to be placed in foster care and exposed to early childhood trauma. |
C.3 BHT Performance Measures
DHCS is developing measures for each of the statewide behavioral health goals in two phases.
-
Phase 1: In June 2025, DHCS published a set of one-time, population-level behavioral health measures, which are defined as measures of community health and wellbeing associated with the statewide behavioral health goals. These population-level measures (sometimes referred to as “Phase 1 Measures”) were limited to publicly available measures with data from 2022-2024 (depending on the measure). They are statewide indicators for which counties are not exclusively responsible; it will take cross-service delivery system collaboration and partnership to move the needle on Phase 1 measures. These measures are listed in Chapter 3, Section E.6 of the Policy Manual.
-
For the first BHSA Integrated Plan (IP), they must be used in the county BHSA planning process and should inform resource planning and implementation of targeted interventions to improve outcomes (additional details on using population-level measures in IPs are in Chapter 3, Section E.6).
-
As part of the 2025 PHM Strategy Deliverable, Medi-Cal MCPs will also use statewide behavioral health goals and measures to inform resource planning and implementation of targeted interventions to improve outcomes.
-
-
Phase 2: In July 2026, DHCS will finalize a list of performance measures (sometimes referred to as “Phase 2 Measures”) that will be used for transparency, planning, population, and accountability purposes and will focus on performance of county behavioral health and Medi-Cal MCPs specifically. Once finalized, BHT performance measures (or “Phase 2 measures”) will replace the population-level behavioral health measures and be used in subsequent county planning and reporting to DHCS, including:
-
The BHSA IP, Annual Updates (AUs) and the Behavioral Health Outcomes, Accountability, and Transparency Report (BHOATR) for county behavioral health; and
-
The annual PHM Strategy Deliverable for Medi-Cal MCPs.
-
DHCS is developing performance measures in consultation with the Quality and Equity Advisory Committee (QEAC), which is comprised of behavioral health, county behavioral health, Medi-Cal MCP, and quality measurement leaders from across California and in partnership with key California state agencies following a three-step process:
-
Identification of the Medi-Cal and BHSA interventions that could advance the goal by developing a “Theory of Change” (a logic model for identifying interventions that research and data suggest will generate a desired impact);
-
Narrowing to the most impactful Medi-Cal and BHSA interventions; and
-
Selection and development of measures for the goal and the most impactful interventions.
The output of the steps above is being shared and discussed in public QEAC meetings throughout calendar years (CY) 2025 and 2026. QEAC meeting materials are available here, and summaries of the Theories of Change will be released later in 2026.
The performance measures fall into the following categories:
-
Goal Measures: Measures of the overall performance on the statewide behavioral health goal for all people enrolled in Medi-Cal or eligible for other county behavioral health services, such as BHSA services. With the exception of the Access to Care, Untreated Behavioral Health Conditions, and Care Experience goals, Goal Measures are multi-stakeholder measures that require coordinated efforts across BHPs, MCPs, and other external partners to advance progress on the goal. Some, but not all, goals also have a Sub-Goal Measure, which generally look at performance on the goal for a sub-population that is most likely to be reached by counties and MCPs or performance on an intermediate outcome anticipated from county and MCP interventions.
-
Intervention Measures: Measures of county and MCP interventions that are most likely to advance progress on each goal.
As noted above in Chapter 2, Section C.2, health equity will be integrated into each of the statewide behavioral health goals. All performance measures will be stratified by key demographics, such as age group and race/ethnicity, and county behavioral health and Medi-Cal MCPs will be expected to address disparities in those measures in their IPs and PHM Strategy Deliverables. In addition, once measures have been developed across all 14 goals, DHCS will identify an additional set of statewide, cross-cutting measures and improvement targets intended to advance equity across all 14 goals. DHCS will finalize these cross-goal equity measures in June 2026.
DHCS expects to revisit performance measures on an ongoing basis, at least every three years, to ensure that they are appropriate and advancing the goals.
C.3.1 How Performance Measures Are Calculated
DHCS will calculate the performance measures using the following data sources:
-
Medi-Cal encounters, claims, enrollment data, and other Medi-Cal data sources;
-
Data collected through Individual Service-Level encounters (including data on BHSA services) submitted by county behavioral health to; and
-
Data shared by other California state agencies, including but not limited to:
-
Homelessness Data Integration System (HDIS) from the California Interagency Council on Homelessness (CalICH);
-
State hospitals data from the California Department of State Hospitals (DSH);
-
Patient Discharge Dataset from the California Department of Health Care Access and Information (HCAI); and
-
Vital Records data from the California Department of Public Health (CDPH).
-
DHCS will publish BHT performance measures, stratified by county behavioral health and Medi-Cal MCPs and by age and key demographics, for public access annually. Via Medi-Cal Connect, a statewide data analytics solution and tool for population health management, DHCS will also provide updated measure calculations and associated underlying data to counties and MCPs as frequently as monthly, depending on the data sources. DHCS does not expect Medi-Cal MCPs or county behavioral health to calculate and submit measures to DHCS.
The first release of performance measures – which is planned for 2026 and is expected to report data from calendar year 2025 – will only include data for Medi-Cal members. Over time, DHCS will integrate data on people not eligible for Medi-Cal who receive behavioral health services from a county (i.e., people eligible for BHSA services).
DHCS will release a BHT Performance Measure Specifications Manual later in 2026 with additional details on how each performance measure is calculated, including the measure specifications.
C.3.2 How BHT Performance Measures Will Be Used
DHCS expects to use performance measures to support Transparency, Planning, Population Health, and Accountability.
Transparency
Performance on all measures, with key stratifications, will be shared with the public and stakeholders on an annual basis.
Planning
DHCS, counties, MCPs, and other stakeholders will use the performance measures to inform their planning for addressing statewide behavioral health goals.
-
Prior to June 2026, counties and MCPs will use the one-time, population-level measures (i.e., Phase 1 measures) to support their community planning process (as outlined in Chapter 3, Section B). Counties will use these population-level measures in their first IP, and MCPs will use these measures in their 2025 PHM Strategy Deliverable.
-
Starting in June 2026, counties and MCPs will transition to using the performance measures (i.e., Phase 2 measures) for all community planning processes and to support data-driven decision making for resource allocation and quality improvement. Counties will use the performance measures beginning with the first AU and for all subsequent IPs and AUs. MCPs will use the latest available performance measures to inform their 2026 PHM Strategy Deliverable and subsequent 2026 PHM Strategy Deliverables.
Population Health
In addition to publishing the performance measures, DHCS expects to provide counties and MCPs with person-level data needed to support appropriate outreach and targeted interventions that would improve outcomes related to each goal.
This person-level data will be provided via Medi-Cal Connect based on role-based access and permissions in accordance with state and federal privacy laws, including, but not limited to, the California Information Practices Act, California GOV Section 11015.5, the Health Insurance Portability and Accountability Act of 1996 (HIPAA), the Privacy Act of 1974, and 42 C.F.R. Part 2 (“Part 2”). For example, MCPs will only receive information on members that are currently assigned to their specific plan, and BHPs will only receive data on individuals with BH needs in their county of responsibility. HSC section 11845.5 is California's SUD privacy law, which imposes stricter requirements than federal substance use treatment laws, does not apply to disclosures made for BHSA-funded services pursuant to WIC section 14197.71(d), provided that the disclosures are authorized under the statute and consistent with federal law, including Part 2.
Data sharing within Medi-Cal Connect is only accessible to authorized Medi-Cal Connect users. DHCS expects that counties and MCPs will be able to share information with their contracted providers for the purpose of outreach and care management, and in accordance with state and federal privacy laws. In the case of Part 2 data, this redisclosure may necessitate additional individual consent. For more information regarding federal and state privacy laws, see the DHCS CalAIM Data Sharing Authorization Guidance.
In addition to providing person-level data in the Medi-Cal Connect platform, DHCS will establish an Application Programming Interface (API) that allows counties and MCPs to ingest individual-level data for the performance measures, including for purposes of integrating with their existing population health management tools and to support measure validation.
Accountability
DHCS will limit the use of performance measures to the three uses above for the first IP period (July 2026 to June 2029) to allow time for counties and MCPs to implement interventions and quality improvement activities after the measures are released.
Over time, and following the first IP period (July 2026 to June 2029), DHCS will have distinct accountability mechanisms for performance measures for BHSA and Medi-Cal. For new DHCS measures, DHCS will allow sufficient time to validate that the data reliably reflects the intent of the measure prior to establishing benchmarks (where relevant) or using the measure for accountability.
BHSA Accountability
DHCS will assess how well counties are addressing the needs of local communities via:
-
Changes in performance measures over time, with consideration for external factors that may influence performance on Goal and Sub-Goal Measures; and
-
BHOATR submissions, which will include a forum for counties to explain their performance on the measures.
DHCS does not plan to issue Corrective Action Plans (CAPs) for performance measures until the second IP period, which begins in July 2029.
Medi-Cal Accountability
Several of the BHT performance measures listed in this document are already monitored in existing Medi-Cal quality and monitoring programs, such as the Managed Care Accountability Set (MCAS), the Behavioral Health Accountability Set (BHAS), Network Adequacy Oversight, and others. Monitoring for these measures will continue in the respective DHCS programs. Beginning with the second IP period (meaning after July 1, 2029), DHCS may add a selection of validated BHT performance measures to these existing Medi-Cal quality and monitoring programs. For example, DHCS may add one or more of the BHT performance measures to BHAS. DHCS would consider Intervention Measures (and not Goal Measures) for inclusion in these quality and monitoring programs, with the exception of Access to Care, Untreated Behavioral Health, and Care Experience, where the Goal Measures may be considered for inclusion in quality and monitoring programs. When considering adding BHT performance measures to quality and monitoring programs, DHCS will follow the standard selection process for these programs, including any applicable stakeholder feedback mechanisms, such as public comment.
BHT performance measures that are added to BHAS and MCAS in the future may be used to determine CAPs and monetary sanctions based on BHAS and MCAS performance.
C.3.3 BHT Performance Measures List
The list below enumerates the BHT performance measures, organized by statewide behavioral health goal. (For the list of one-time, population-level measures used only for the first IP, see Chapter 3, Section E.6.). Performance measures labeled as DHCS Measure indicate a new measure that DHCS has developed as part of the BHT performance measure set (sometimes referred to as “Phase 2 Measures”).
1-3. Improving Access to Care, Reducing Untreated Behavioral Health Conditions, and Improving Care Experience
-
One or More BH Services for People with MH Needs – DHCS Measure
-
One or More BH Services for People with Significant MH Needs – DHCS Measure
-
Initiation of SUD Treatment (IET-I) – NCQA Measure
-
One or More BH Services for People with Significant MH Needs and Co-Occurring SUD – DHCS Measure
-
Three or More BH Services for People with MH Needs – DHCS Measure
-
Three or More BH Services for People with Significant MH Needs – DHCS Measure
-
Engagement in SUD Treatment (IET-E) – NCQA Measure
-
Three or More BH Services for People with Significant MH Needs and Co-Occurring SUD – DHCS Measure
-
Perception of Care with Respect to One's Cultural Background: SMHS – UCLA ISP and SAMHSA Measure
-
Perception of Care with Respect to One's Cultural Background: DMC-ODS – UCLA ISP and SAMHSA Measure
-
Perception of Care with Respect to One's Cultural Background: NSMHS – MCP CAHPS Measure
-
Depression Screening and Follow-Up for Adolescents and Adults (DSF-E) – NCQA Measure
-
Evidence-Based Practices for People Living with Significant MH Needs – DHCS Measure
-
Follow-Up After Emergency Department Visit for Substance Use (FUA) – NCQA Measure
-
Follow-Up After Emergency Department Visit for Mental Illness (FUM)– NCQA Measure
-
Improving Prevention & Treatment of Co-Occurring Physical Health Conditions
-
Ambulatory Services for Adults with Significant BH Needs – DHCS Measure
-
Well Child Visits for Children and Youth with Significant BH Needs – DHCS Measure
-
Dental Visits for People with Significant BH Needs – DHCS Measure
-
Reducing Homelessness
-
Homelessness Among People with Significant BH Needs – DHCS Measure
-
Permanent Housing for People with Significant BH Needs Who Experience Homelessness – DHCS Measure
-
Housing Services for People with Significant BH Needs Who Experience Homelessness – DHCS Measure
-
Full Service Partnership and Housing Services for People with Significant BH Needs Who Experience Homelessness – DHCS Measure
-
Reducing Institutionalization
-
Institutional Stays for People with BH Needs – DHCS Measure
-
Coordinated Specialty Care for First Episode Psychosis – DHCS Measure
-
Support for Transitions from Institutional BH Care – DHCS Measure
-
Follow-Up After Hospitalization for Mental Illness (FUH) – NCQA Measure
-
Follow-Up After Other Institutional Stays for Behavioral Health – DHCS Measure
-
Reducing Justice Involvement
-
Justice-Involvement Among People with Significant BH Needs – DHCS Measure
-
Repeat Justice-Involvement Among People with Significant BH Needs – DHCS Measure
-
Post-Release BH Services for Justice-Involved People with Significant BH Needs – DHCS Measure
-
Continuation of MAT for Justice-Involved Reentry Enrollees – DHCS Measure
-
Reducing Overdoses
-
Deaths by Drug Overdose – DHCS Measure
-
Repeat ED Visit or Hospitalization for Drug Overdose – DHCS Measure
-
Contingency Management – DHCS Measure
-
Pharmacotherapy for Opioid Use Disorder (POD) – NCQA Measure
-
Follow-Up After High-Intensity Care for Substance Use Disorder (FUI) – NCQA Measure
-
Reducing Removal of Children from Home
-
Children and Youth in Foster Care – DHCS Measure
-
BH Services for Children and Youth in Foster Care – DHCS Measure
-
BH Services for Parents, Guardians, and Pregnant People with Significant BH Needs – DHCS Measure
-
High Fidelity Wraparound, Enhanced Care Management, or Intensive Care Coordination for Children and Youth in Foster Care – DHCS Measure
-
Reducing Suicides
-
Deaths by Suicide – DHCS Measure
-
Repeat ED Visit or Hospitalization for Self-Harm – DHCS Measure
-
Follow-Up MH Services After Crisis Services – DHCS Measure
Proposed measures for the following four Statewide Behavioral Health Goals will be developed in Q1-Q2 2026:
-
Improving Engagement in School
-
Improving Engagement in Work
-
Improving Social Connection
-
Improving Quality of Life
